Specialty Areas

A normal, healthy spine provides balance and supports the body’s weight. On the other hand, a spinal deformity – or an abnormal alignment or curve of the vertebral column – can throw that balance off.
Spinal deformity can happen in a number of different ways, the most prevalent being the result of a birth defect, aging, injury, or previous spine surgery.
Types
Scoliosis is a side-to-side curvature of the spine that can develop in adults when their facet joints and discs begin to deteriorate. The facet joints give the spine flexibility, enabling us to twist, stretch, or curl up on the couch. When these joints deteriorate, the spine bones can tilt and begin to shift to one side
Kyphosis is an abnormal forward rounding of the spine of more than 50 percent. In the upper (thoracic) back, kyphosis is typically due to osteoporotic compression fractures. Kyphosis can also occur in the lower back (lumbar) spine. The disorder limits function and doesn’t allow the sufferer to stand up straight.
Lordosis, or swayback, is a condition in which the spine curves significantly inward at the lower back, giving a backward leaning appearance.
Adult scoliosis and kyphosis can be caused by age-related wear and tear on the back or complications from past spine surgeries. Moderate deformities occur when the facet joints and discs deteriorate over time and are no longer able to support the spine’s normal posture. The cause of lordosis is unknown, but is generally associated with poor posture, a congenital problem with the vertebrae, neuromuscular problems, back surgery, or a hip problem.
Symptoms
Pain is one of the most prevalent symptoms of a spinal deformity, resulting from stressed joints and pinched nerves, not the abnormal curve. The stretching and compression of the spinal cord or nerve roots caused by the deformity produces symptoms that may include pain, weakness, numbness, or tingling that travel down an arm or a leg.
Treatment
Generally speaking, non-invasive, non-operative treatments will be recommended before surgery is considered. These treatments include pain medications, physical therapy, and sometimes bracing.
Dr. Reto may recommend surgery if:
- There is severe pain not relieved by non-invasive treatments
- The spinal deformity is progressing
- The physical deformity is unbearable
- Compression of the spinal cord or nerve roots has occurred
- Fractures have occurred
The goals of surgery are to relieve symptoms and to align and stabilize the spine. Dr. Reto will discuss surgical options with you and will recommend the one he believes is best for your individual circumstances.

DEGENERATIVE SPINE DISEASES
Dr. Reto is a recognized leader in the treatment of degenerative spine conditions, which are typically caused by age-related wear and tear.
Degenerative changes can occur almost anywhere along the spine and can affect the structures of the spine, including:
Discs – The soft, gel-like pads located between the vertebrae and function as shock absorbers when you flex, rotate, or bend your back or neck.
Vertebrae – The hard bones of the spine are called vertebrae and house and protect the spinal column and nerves.
Ligaments, Tendons, and Cartilage – These structures connect the bones of the spine and aid in joint stability.
Types
Degenerative Disc Disease
As we age, the discs may thin to the point where there is insufficient padding between vertebrae. At the same time, the outer layer of the spine can develop cracks, which gradually worsen. The discs may also develop herniated areas, which is where the central portion of the disc protrudes through the outer layer. Symptoms include pain, tingling, numbness, or weakness in the neck, arms, hands, back, hips, or legs, depending on where along the spine the disc degeneration occurs.
Myelopathy
Myelopathy is the undue pressure on your spine due to compression of the spinal cord. As a person ages, several things can start to happen:
- The discs between the vertebrae start drying out and begin to bulge or herniate.
- The shape of the vertebrae changes due to arthritis, causing spur-like protrusions.
- The ligaments linking your vertebrae thicken.
Due to a combination of these factors, the spinal canal narrows, eventually leading to pressure on the spinal cord and myelopathy. Symptoms include pain, tingling, or numbness in the arms or legs; difficulties with coordination, walking, and fine motor skills; a feeling of heaviness in the extremities.
Radiculopathy
Radiculopathy occurs when a nerve root along the spine becomes inflamed or damaged, causing pain and other symptoms in the arm/shoulder/hand area or the buttock/leg/foot area. Radiculopathy most commonly results from degenerative changes to the spine over long periods of time but can also occur due to acute injury or illness. Symptoms can include pain, numbness, weakness, tingling, and altered reflexes.
Stenosis
Spinal stenosis is the thickening of the ligaments, formation of bone spurs, and deterioration of the disc material. As a result, the spinal canal narrows and pinches the nerve. The bone spurs may also press on the spinal cord. Symptoms can include pain in the back or neck, radiating pain into the legs or arms, and difficulty standing or walking.
Treatment
Many people with degenerative spine disease respond well to conservative, non-surgical treatment. This conservative treatment typically includes anti-inflammatory medication and pain relievers. Physical therapy can help to manage your symptoms and may include manual therapy, heat and other pain-relieving methods, stretching, strengthening exercises and education to help you manage your condition.
For a small group of people who don’t respond to conservative treatment, surgery may be necessary, particularly if there are signs and symptoms of nerve compression or joint instability. There is a wide range of surgical techniques that can be used, depending on the extent, location, and exact nature of the degeneration. Dr. Reto will make sure you understand your surgical options and will work with you to develop an individualized treatment plan.
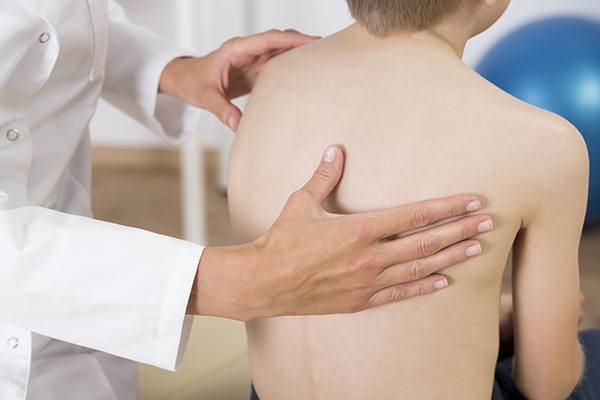
SCOLIOSIS
Scoliosis is an abnormal curvature of the spine that typically occurs during the growth spurt just before puberty, between the ages of 10 – 12, although some types of scoliosis appear much sooner.
Most cases of pediatric scoliosis are mild and don’t require treatment, but some children develop spine deformities that get worse as they grow and must be treated.
Adult scoliosis is typically the result of untreated childhood scoliosis, but it also may result from a degenerative joint condition. Symptoms include pain and stiffness in the lower back; numbness, cramping, or shooting pain in the legs; fatigue due to unusual strain on muscles, back, and legs.
Severe scoliosis can be disabling. An especially severe spinal curve can reduce the amount of space within the chest, making it difficult for the lungs to function properly.
Types
There are several types of scoliosis that occur in children and adults:
- Congenital scoliosis occurs before birth when the spine doesn’t form, correctly.
- Early-onset scoliosis appears between birth and 10 years of age.
- Adolescent idiopathic scoliosis occurs as a child grows older and manifests as a curving and twisting of the spine.
- Degenerative scoliosis affects adults through the wear and tear of the skeletal system.
- Neuromuscular scoliosis occurs when there is a problem with the muscles or nervous system.
- Syndromic scoliosis occurs due to any number of syndromes, including Marfan’s syndrome, Beal’s syndrome, and trisomy 21.
Treatment
When scoliosis appears in children, treatment often isn’t necessary because the curve typically corrects itself as the child grows. However, checkups are recommended every four to six months.
Dr. Reto typically recommends one or a combination of three types of treatments:
Observation & Monitoring
We generally recommended this option for children and adolescents whose curvatures are small or moderate. For adults, we will recommend observation, exercise, and physical therapy if the curves are not large, combined with the judicious use of non-steroidal anti-inflammatory medications.
Bracing
A brace is especially helpful for children with moderate scoliosis whose bones have stopped growing. Although wearing a brace won’t cure scoliosis or reverse the curve, it can prevent further curve progression. The more hours a day the brace is worn, the more effective it is.
Surgery
A small number of scoliosis patients will require surgery. That’s because severe scoliosis typically gets worse over time unless surgically treated. Dr. Reto typically uses less invasive surgical techniques that translate to gold standard outcomes, but with quicker recovery and less pain for the patient.

FAILED BACK SYNDROME
Unfortunately, not all back surgeries result in complete pain relief. A small percentage of patients will discover they still have back pain as they recover or find they have new pain. Failed back syndrome is the general term used to describe this condition.
Failed back syndrome doesn’t necessarily mean your surgery truly “failed” in the medical sense; it may have been that the surgery uncovered unknown issues that resulted in more pain.
Treatment
For patients who have failed back syndrome, treatment starts with a complete diagnosis that utilizes high tech imaging as well as a thorough exam. Once Dr. Reto has determined the cause of the continued pain, he will develop a treatment plan that may include nonsurgical or surgical methods.
Nonsurgical
It is possible to treat some forms of failed back syndrome with nonsurgical methods such as medication and physical therapy. If this is possible, this will be the first line of defense.
Surgical
If surgery is required, it may include hardware removal or replacement, specific fusions, or a number of other different procedures that are designed to ease your pain.